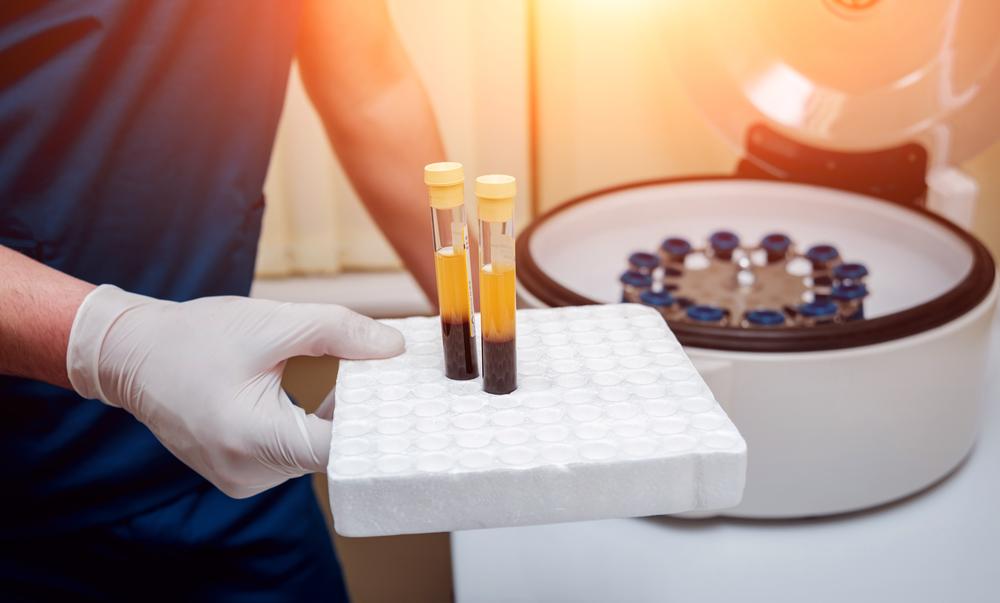
In the last few decades, advances in regenerative medicine have been made in a variety of medical specialties, most notably orthopedics. Stem cell therapy is becoming an increasingly popular treatment option for patients with degenerative conditions such as arthritis, chronic pain, and other joint pain. By encouraging the healing and regeneration of some damaged tissues, such as cartilage in the joint, these treatments may be able to help restore some physical functions.
Platelet-rich plasma therapy uses the blood’s own natural healing properties to promote the healing of tendons, muscles, ligaments, and cartilage, as well as bone, in some cases. What is your level of familiarity with these methods of treating joint discomfort? Continue reading to find out more.
Table of Contents
Stem Cell and Plasma Therapy
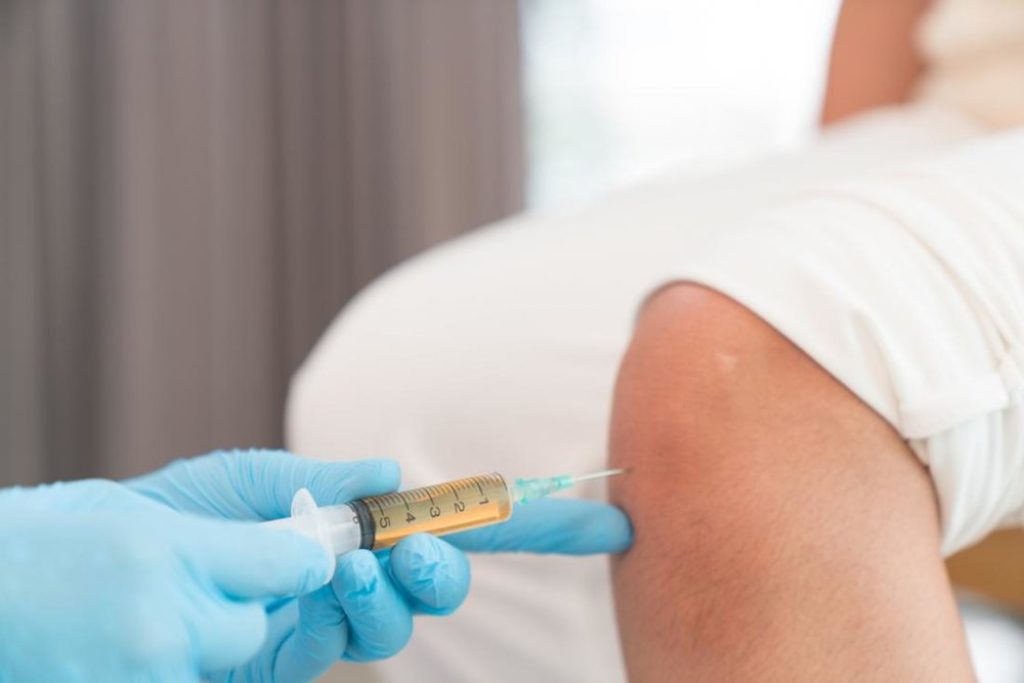
Source: tehrantimes.com
Stem cells are often referred to as “the body’s handyman,” and they are usually plentiful in an otherwise healthy individual. Stem cell therapy is used to treat a variety of conditions, including cancer, organ damage, and joint pain. These cells are known to treat inflammation, which is a source of pain in many conditions, as well as encourage restorative healing by adopting the characteristics of the cells in the area of the body being treated. By making use of the body’s own healing source and mechanisms, most stem cell therapies do not come with negative side effects.
Platelet-rich plasma therapy is a type of stem cell regimen used to treat cartilage damage (PRP). As a result of the cells being derived from the patient’s own blood, the treatment has no known side effects. Blood plasma is the fluid component of the blood that transports red and white blood cells throughout the body. Even though it’s primarily water, it also contains a variety of nutrients such as proteins, glucose, and antibodies. When blood clots, platelets play a role in the process, as they aid in the formation of the clot. However, they produce a substance called “growth factor” that governs normal healing and growth and stimulates tissue to heal itself.
Presently, there is no standard definition of what constitutes “platelet-rich plasma,” so the patient should be aware of the differences between the various types of therapy he or she might be receiving. Variations in the types of compounds used in therapies can result from differences in blood composition of the patient, how the blood sample derived from the patient is processed, and what additives are added to the compound to facilitate further healing. It is also imperative to do your research on the administering physician to ensure they are qualified to do so, a good example of one would be Dr. Brian Gruber at Integrated Orthopedics.
How it works
The mechanisms of action of stem cells and platelet-rich plasma are still unknown to medical researchers. However, some observations regarding patients who have received the therapies note the following:
- Stimulation of new cartilage formation
- Reduces inflammation
- Slows the progress of arthritis
- Stimulates the natural production of joint lubricating fluid, easing friction in the joints
- Alleviates pain due to tendonitis, bursitis and muscle strain.
While these results are not universal for every patient, in general, patients who have made use of the therapies have experienced positive results and some alleviation of symptoms. Medical professionals do stress, however, that more clinical trials and observation will be needed to definitively state the viability of stem cell and platelet-rich plasma therapies.
The Process
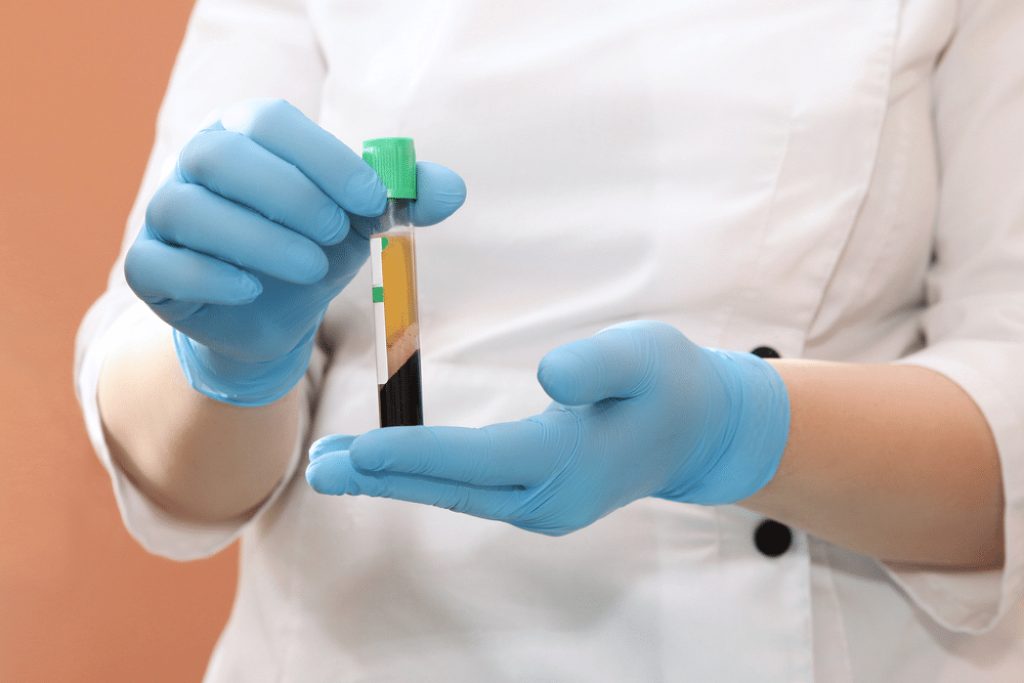
Source: rightpathpainandspine.com
Because each person’s body chemistry differs from another’s, the compound used in platelet-rich plasma therapy is derived from the patient’s own blood. Also, different physicians might utilize varying techniques to prepare the PRP solution. As a regimen for cartilage repair, is not yet recognized by the FDA and medical experts, there are also no current standard guidelines for how the remedy is used. However, generally, a patient can expect the following in a course of PRP therapy:
The PRP Solution is Compiled
In preparing the solution to be used in the therapy, the patient first gives a blood sample that is then placed in a medical centrifuge where its high speed separates the blood components. Blood is usually composed of around 45% red blood cells, while white blood cells and platelets make up around 1%, and plasma makes up the rest, roughly around 55%. Once this separation process is completed, the technician will then prepare the components for PRP injection. The goal is to create a solution that has around three times the normal density of platelets per microliter of normal blood (150K to 450K). Some doctors choose to include additives in this solution that serve to activate the platelets and boost regenerative properties.
Results of PRP therapy
Source: prpstemcellinphilly.com
Once the PRP has been created, it is injected into the joint at the site of discomfort. In one study published in 2013, patients with knee osteoarthritis took part in a study in which some patients received injections with PRP solutions and some received placebos. The patients who were given the actual solution reported a reduction in pain and improved knee function after several weeks. Those treated with placebos reported no change or slight increases in pain and decreased joint functionality.
These therapies do not always work for everyone, however. Some studies indicated that those who received the injections did not fare better than their placebo groups, though the studies do indicate that differences in preparation of the solution might have played a role in these results. There is also some thought towards patients receiving multiple PRP solution doses for it to be more effective, and that is likely these therapies are best paired with other therapies, such as physical therapy.
Pros and Cons
Patients should fully inform themselves about any therapies recommended by their doctors, and decide on their own if the treatment is right for them. With that in mind, consider some of the following advantages and disadvantages of PRP therapy.
PROS:
- As the solution is derived from the patient’s own body, there are fewer issues with rejection and side effects.
- Does not negatively impact the tissue in the long run as cortisone injections are known to do.
- No known long-term effects in pain reduction as are common in anti-inflammatory medications.
CONS:
- The process is not yet FDA-approved and might not be covered by insurance.
- Results can vary due to different techniques and a lack of standardization in solution preparation.
- Lack of clinical trials on the process means it is uncertain if the therapy is contraindicated in certain conditions, if certain additives are needed to make it more effective, or at what frequency they should be given.
What to Expect

Source: austinorthobio.com
Stem cell and platelet-rich plasma therapies are outpatient procedures, and usually do not last longer than an hour. As with any injection, the pain of this procedure should be limited to just the discomfort of the injection itself. The majority of patients can return to their daily routines immediately following treatment, but it is important to stress that each patient’s response to treatment varies. After the therapy, if any symptoms are alleviated, it is usually within a short period of time, and in some cases, immediately. If a patient agrees to participate in a clinical trial for the treatment, they may be able to get their medical care paid for.
Doctors who perform PRP therapy should be evaluated on how they assess the problem, what methods of diagnosis they use, and how much training they have in preparing and administering PRP therapy. The doctor should go over with the patient, before the treatment, the possible benefits and risks of the procedure, the follow-up protocol, and the cost of the procedure, especially if it is not covered by insurance.
As the treatment is considered experimental by most insurance companies, patients will often end up paying out of pocket for the procedure, which can cost anywhere between $500 and $2,000. Although the American Academy of Orthopedic Surgeons doesn’t clearly define who is eligible for the therapy, it is generally agreed upon as a viable option for patients who have found that their pain has limited their daily activities, have a sensitivity to anti-inflammatory medications, have not found relief with or want to avoid steroid injections, and have shown signs of the condition worsening.
Platelet transfusions may not be suitable for those with bleeding disorders (such as hemophilia), pregnancy, anemia, or other medical conditions that could be exacerbated by the introduction of more platelets into the bloodstream, such as metastatic diseases.







