
The novel coronavirus (COVID-19) outbreak is close to completing a year on planet Earth. However, it is far from disappearing from our lives. Various parts of the world are having a firsthand experience of these effects, where the virus keeps coming back in waves.
In Canada, the virus first peaked during the month of May, where it overwhelmed healthcare systems and professionals throughout the country. Personal protective equipment (PPE) proved challenging to obtain, and additional support for COVID-19 patients became hard to find.
During that time, when healthcare professionals weren’t busy treating patients, they were scrambling to repurpose PPE to protect themselves on the frontlines of COVID-19.
As the novel coronavirus makes its way back to Canada, it has come with almost double the force of the highest daily cases recorded previously. This calls for intensive preparation of PPE, especially critical items such as the N95 mask.
Due to this reason, those who work in the healthcare sector have crucial questions about the times ahead. One of the most pressing inquiries relates to the N95 respirator, specifically the ability to reuse it read now.
Table of Contents
Can You Reuse an N95 Mask?

img source: health.com
Under normal circumstances, N95 respirators are meant to be worn only once per use session. This translates to consistent or recurring usage over a period of several hours. After this, it’s advised that you discard your mask and wear a new one to cover your nose and mouth from respiratory exposure.
However, in emergency use cases where there is a shortage of PPE, you can repurpose or reuse the mask after taking relevant safety measures. This is something that should only be done as a last resort, where you or your facility is running short on your mask supply and cannot find new masks due to a crisis.
The Respirator Degrades With Consistent Use
This precaution to avoid reusing the N95 respirator is due to the mask’s overall structure, design, and functionality.
Since the N95 is a filtering facepiece respirator (FFR), it uses its overall structure and material to clean the surrounding air before the wearer could breathe it in.
The particulate filter material of the mask cleans the air from external particles such as viral agents. Whereas, the professionally-fitted mechanism creates a seal around the face and ensures that contaminated air doesn’t seep in through the edges.
With this mechanism, the N95 mask decontaminates the surrounding air from at least 95 percent of foreign agents such as dust, mists, and fumes. This also includes the virus that causes COVID-19. As a result, the air intake by the wearer remains massively clear of harmful particles.
However, when the wearer consistently uses the mask in a contaminated environment such as a COVID-19 treatment room, it can degrade the equipment’s overall strength with time. Taking the mask off for meal breaks or bathroom visits further affects its fit and puts the wearer’s safety at risk.
In non-medical settings such as moderate exposure to dust particles, the N95 FFR can last up to 8 hours of usage. But in medical settings such as high exposure to COVID-19, there is no specific limit of hours that defines how long you can use the respirator.
That’s why medical experts advise that healthcare workers dispose of the mask after using it for a few hours to ensure ideal protection. Otherwise, putting the mask on and pulling it off multiple times can massively reduce the protection it offers.

img source: rocketcdn.me
Health Canada Has Provided Guidelines for Repurposing These FFRs
During the initial wave of the COVID-19 outbreak, Health Canada took notice of the mask shortage and provided guidelines to repurpose N95 respirators. These advisories still stand and can be put into place if you are facing a shortage of PPE.
With that being said, it is highly critical to understand that decontaminating your N95 mask doesn’t make it good as new. It still works, but with compromised performance. That is why you need to make sure that if you can obtain new respirators, you don’t take the route of repurposing older ones.
Keeping that in mind, here are a few guidelines on how to reuse your N95 FFRs safely under crisis.
Use Specialized Protocols to Decontaminate FFRs
img source: hpnonline.com
According to Health Canada, you can use specialized equipment to decontaminate your N95 respirators. These solutions are labeled as Class II medical devices and need proper regulation from the authorities to be fit for this application.
You can also use vaporized hydrogen peroxide (VHP) with concentrations above 30 percent. While multiple studies have mentioned that these measures were successful, it’s important to bear in mind that the data isn’t enough to be followed without precautionary measures.
Rotate Respirators Through Multiple Shifts
Apart from decontamination, one strategy is to rotate your N95 respirators throughout your patient treatments. This requires more than one respirator at hand, which can go about five respirators per person. But this particular step ensures that you steer clear of an increased risk of contracting COVID-19.
According to Health Canada, the virus that causes COVID-19 can live on plastic surfaces for up to three days. As a result, waiting to reuse your N95 mask for three days from its last donning can reduce the risk of catching an infection through it.
Know the Limits to Reuse Your Masks
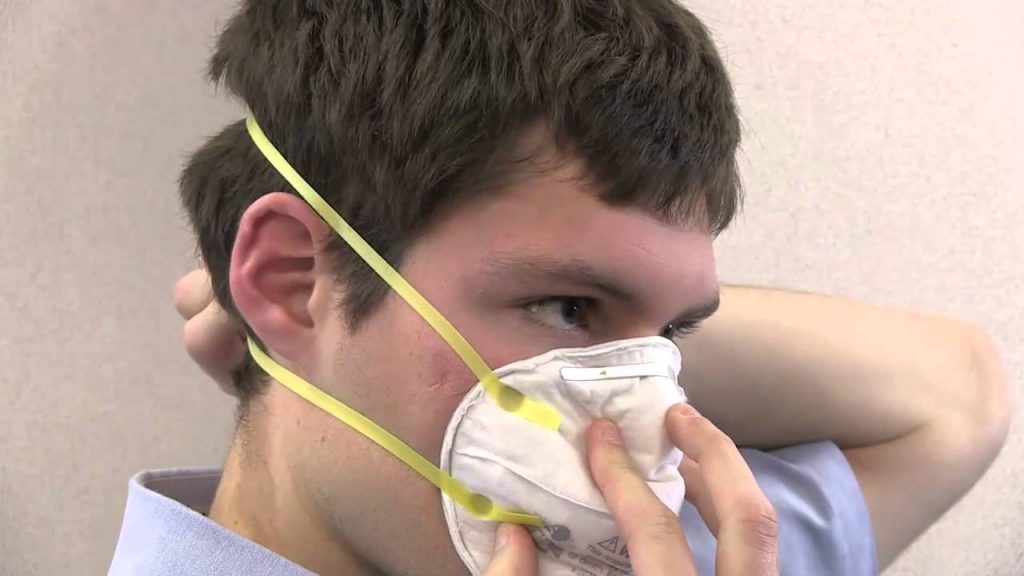
img source: youtube.com
As a rule of thumb, you should not reuse your FFR more than five times per piece. It’s because if you put on your mask multiple times, it can eventually have an effect on its overall fit. This could directly hinder its ability to protect you.
Similarly, you should never reuse a mask that has splashes or splatter of blood or bodily fluids on it. In order to reduce this overall exposure and the risk that comes with it, you can consistently pair your masks with a face shield.
It’s Important to Only Reuse Your PPE Under Crisis
While these strategies can help mitigate your risk and allow you to reuse your N95 FFRs, you should make it a point to buy new respirators whenever possible. This makes sure that you are able to protect yourself and your team members through COVID-19 treatment settings without compromising anyone’s safety.







